Fentanyl addiction, clinically diagnosed as opioid use disorder involving fentanyl, develops when repeated exposure to this synthetic opioid produces rapid physical dependence and compulsive drug-seeking behavior.
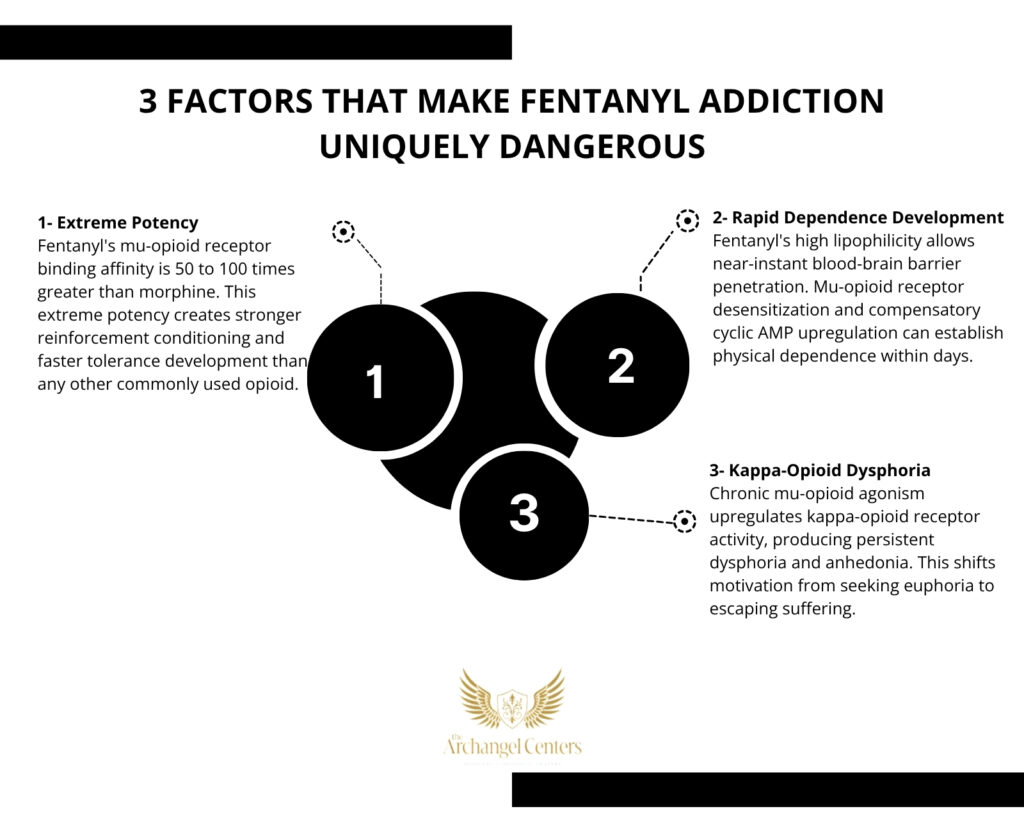
Fentanyl is approximately 50 to 100 times more potent than morphine, meaning tolerance, dependence, and addiction can develop faster than with any other commonly used opioid.
What separates fentanyl from other opioids is the extremely narrow margin between a dose that produces euphoria and a dose that causes fatal respiratory depression. As little as 2 milligrams of fentanyl can be lethal depending on the individual.
Understanding how fentanyl hijacks the brain’s opioid system is essential for recognizing the signs of addiction early and accessing treatment that addresses both the physical dependence and psychological drivers of compulsive use.
Key Takeaways
- According to CDC provisional data, overdose deaths involving synthetic opioids (primarily fentanyl) decreased from over 76,000 in 2023 to approximately 48,000 in 2024, though fentanyl remains the leading driver of drug overdose mortality in the United States.
- Fentanyl’s high lipophilicity allows rapid penetration of the blood-brain barrier, producing onset of effects within seconds when injected or smoked and creating stronger reinforcement conditioning than slower-acting opioids.
- SAMHSA reports that 80% of people who needed substance use disorder treatment in 2024 did not receive it, highlighting the critical gap between need and access for opioid use disorder.
- FDA-approved medications for opioid use disorder, including buprenorphine (Suboxone), naltrexone (Vivitrol), and methadone, significantly improve treatment retention and reduce overdose mortality when combined with behavioral therapy.
Understanding Fentanyl and Opioid Use Disorder
Fentanyl addiction is classified as opioid use disorder (OUD) in the DSM-5-TR, a chronic medical condition characterized by compulsive opioid use, inability to control intake, and continued use despite harmful consequences.
What Is Fentanyl?
Fentanyl is a fully synthetic opioid originally developed in 1960 for surgical anesthesia and severe pain management, now classified by the DEA as a Schedule II controlled substance.
Key pharmacological properties of fentanyl include:
- Fentanyl binds to mu-opioid receptors with binding affinity approximately 50 to 100 times greater than morphine, producing profound analgesic and euphoric effects at microgram-level doses.
- Fentanyl detection windows vary significantly by testing method, with urine tests detecting the drug for 7 to 19 days in regular users, blood tests for approximately 12 hours, and hair follicle tests for up to 90 days.
- The drug’s high lipophilicity enables rapid penetration of the blood-brain barrier, reaching peak brain concentration within seconds when injected and within minutes when smoked or nasally insufflated.
- Illicitly manufactured fentanyl (IMF) now dominates the illicit opioid supply in the United States, frequently pressed into counterfeit pills designed to mimic oxycodone, alprazolam, and other prescription medications.
DSM-5-TR Diagnostic Criteria for Opioid Use Disorder
The DSM-5-TR defines opioid use disorder through eleven diagnostic criteria, requiring a minimum of two within a 12-month period, with severity stratified from mild to severe.
Core diagnostic indicators include:
- Taking fentanyl or other opioids in larger amounts or over longer periods than intended, reflecting the loss of dosing control driven by escalating tolerance and physical dependence.
- Continued opioid use despite knowledge of persistent physical or psychological problems caused or exacerbated by the substance, including respiratory complications and mood disturbances.
- Withdrawal symptoms when fentanyl use is reduced or stopped, or using fentanyl (or a pharmacologically similar opioid) to relieve or avoid withdrawal, confirming physiological dependence.
- Craving or strong urge to use opioids, representing the conditioned motivational state that drives relapse vulnerability even during periods of sustained abstinence.
Fentanyl Potency Compared to Other Opioids
Fentanyl’s extreme potency relative to other opioids fundamentally changes the risk profile for both dependence development and overdose mortality.
Potency comparisons include:
| Opioid | Approximate Potency Relative to Morphine | Typical Lethal Dose Range |
|---|---|---|
| Morphine | 1x (reference) | 200+ mg |
| Heroin | 2 to 5x | 75 to 375 mg |
| Oxycodone | 1.5x | 80+ mg |
| Fentanyl | 50 to 100x | 2 mg |
| Carfentanil | 10,000x | 20 mcg |
- This extreme potency means dosing errors measured in micrograms can produce fatal respiratory depression, particularly in opioid-naive individuals who encounter fentanyl unknowingly in counterfeit pills or adulterated drug supplies.
- Fentalogs (novel fentanyl analogs) including acetylfentanyl, furanylfentanyl, and para-fluorofentanyl vary unpredictably in potency and duration, further complicating both use and emergency response.
How Fentanyl Hijacks the Brain
Fentanyl produces its addictive effects through powerful activation of the brain’s endogenous opioid system, triggering neuroadaptations that create physical dependence more rapidly than most other opioids.
Mu-Opioid Receptor Activation
Fentanyl functions as a full agonist at mu-opioid receptors (MOR), producing maximal receptor activation at the molecular level and generating the strongest possible opioid signal.
Mu-opioid receptor effects include:
- Fentanyl binding to MOR in the ventral tegmental area triggers dopamine release in the nucleus accumbens, producing intense euphoria that reinforces drug-seeking behavior through mesolimbic pathway activation.
- Simultaneously, MOR activation in the brainstem respiratory centers depresses breathing rate and tidal volume, creating the direct mechanism through which fentanyl overdose produces fatal respiratory arrest.
- Fentanyl’s high receptor binding affinity and rapid onset produce stronger reinforcement conditioning compared to slower-acting opioids, accelerating the transition from use to dependence.
Tolerance and Physical Dependence
Chronic fentanyl exposure triggers homeostatic adaptations in opioid receptor signaling that produce both tolerance and physical dependence within days to weeks of regular use.
Neuroadaptive changes include:
- Mu-opioid receptor desensitization and internalization reduce receptor availability on cell surfaces, requiring higher fentanyl doses to achieve the same analgesic and euphoric effects.
- Compensatory upregulation of the cyclic AMP signaling cascade produces a state of neuronal hyperexcitability that manifests as opioid withdrawal symptoms when fentanyl is reduced or discontinued.
- Locus coeruleus hyperactivity during withdrawal generates the characteristic noradrenergic storm producing anxiety, muscle pain, diaphoresis, lacrimation, rhinorrhea, and gastrointestinal distress.
The Role of Kappa-Opioid Dysphoria
Beyond the mu-opioid system, chronic fentanyl use dysregulates kappa-opioid receptors (KOR), contributing to the dysphoria and negative emotional states that drive compulsive use.
Kappa-opioid effects include:
- Chronic mu-opioid agonism produces compensatory upregulation of kappa-opioid receptor activity, generating persistent dysphoria, anhedonia, and stress sensitivity during periods without fentanyl.
- This kappa-opioid-mediated negative emotional state transforms the motivation for fentanyl use from positive reinforcement (seeking euphoria) to negative reinforcement (escaping dysphoria), a shift that characterizes advanced opioid use disorder.
- Kappa-opioid dysphoria persists beyond acute withdrawal, contributing to the protracted withdrawal syndrome that threatens relapse for months after physical detoxification is complete.
How Fentanyl Dependence Develops
Opioid use disorder involving fentanyl develops through a predictable neurobiological progression accelerated by the drug’s extreme potency and rapid onset of action.
Initial Exposure and Rapid Reinforcement
First exposure to fentanyl, whether intentional or through contaminated drug supply, produces immediate and powerful opioid reinforcement.
Early exposure patterns include:
- Fentanyl’s rapid blood-brain barrier penetration produces peak euphoria within seconds to minutes, creating stronger associative conditioning than slower-onset opioids like oral oxycodone or hydrocodone.
- Many individuals first encounter fentanyl unknowingly through counterfeit pills or adulterated heroin, cocaine, or methamphetamine, bypassing the gradual dose escalation that characterizes traditional opioid use disorder progression.
- The intensity of initial fentanyl effects can establish tolerance-driving neuroadaptations after only a few exposures, particularly in opioid-naive individuals whose receptor systems have no prior adaptation.
Escalation and Cross-Tolerance
As tolerance develops, individuals require progressively higher fentanyl doses or more frequent administration to achieve baseline opioid effects.
Escalation characteristics include:
- Cross-tolerance between fentanyl and other opioids means individuals transitioning from prescription opioids or heroin to fentanyl may initially tolerate higher doses, but the unpredictable potency of illicit fentanyl eliminates this protective margin.
- The transition from intermittent to daily use typically accelerates once physical dependence establishes, as withdrawal avoidance becomes a stronger motivator than euphoria-seeking behavior.
- Financial burden escalates rapidly as tolerance increases, often precipitating criminal activity, loss of employment, and dissolution of family and social support structures.
Risk Factors for Fentanyl Use Disorder
Specific biological, environmental, and exposure-related factors determine individual vulnerability to developing opioid use disorder involving fentanyl.
Primary risk factors include:
- Prior prescription opioid use or misuse significantly increases risk, with individuals prescribed opioids for chronic pain representing a substantial proportion of those who transition to illicit fentanyl use.
- Co-occurring mental health conditions including major depressive disorder, post-traumatic stress disorder, and generalized anxiety disorder increase opioid use disorder risk through self-medication pathways.
- Genetic factors influencing mu-opioid receptor expression, opioid metabolism, and reward sensitivity account for approximately 40% to 60% of opioid addiction vulnerability.
Signs and Symptoms of Fentanyl Addiction
Fentanyl addiction produces characteristic opioid intoxication signs, withdrawal symptoms, and behavioral changes that intensify as the severity of use disorder progresses.
Common Signs of Fentanyl Use
The most recognizable indicators of fentanyl use reflect the drug’s depressant effects on the central nervous system and respiratory function.
Physical signs of active fentanyl use include:
- Pinpoint pupils (miosis), drowsiness or sedation alternating with periods of alertness (“nodding”), and slowed or shallow breathing represent the classic triad of opioid intoxication.
- Constipation, nausea, decreased appetite, and dry mouth occur with regular fentanyl use due to opioid receptor activation throughout the gastrointestinal tract.
- Track marks from injection use, nasal irritation from insufflation, or burns on lips and fingers from smoking fentanyl on foil indicate specific routes of administration.
Behavioral indicators include:
- Social withdrawal, loss of interest in previously valued activities, and increasing secrecy around daily schedule and finances suggest progressive opioid use disorder.
- Doctor shopping, forging prescriptions, or purchasing pills from non-medical sources indicates escalating dependence and loss of controlled access.
- Alternating between periods of euphoric sedation and anxious, irritable withdrawal states creates an observable mood cycling pattern that correlates with dosing schedule.
Severe Symptoms and Overdose Recognition
Fentanyl’s extreme potency produces severe complications that can progress to fatal overdose within minutes, requiring immediate emergency response.
Severe complications and overdose indicators include:
- Respiratory depression progressing to respiratory arrest is the primary mechanism of fentanyl overdose death, with breathing rate falling below 8 breaths per minute indicating a life-threatening emergency requiring immediate naloxone (Narcan) administration.
- Loss of consciousness, unresponsiveness to stimulation, and blue or purple discoloration of lips and fingertips (cyanosis) signal inadequate oxygenation requiring emergency intervention.
- Fentanyl-induced muscle rigidity, particularly involving the chest wall (“wooden chest syndrome”), can physically prevent adequate ventilation even with assisted breathing, representing a complication unique to potent synthetic opioids.
Long-Term Effects of Chronic Fentanyl Use
Sustained fentanyl use produces progressive physiological damage and deepening psychological dependence that complicate long-term recovery.
Long-term consequences include:
- Chronic opioid-induced hormonal disruption (opioid endocrinopathy) reduces testosterone, estrogen, and cortisol production, causing sexual dysfunction, osteoporosis, depression, and immune suppression.
- Opioid-induced hyperalgesia, a paradoxical increase in pain sensitivity caused by chronic opioid receptor activation, worsens the very pain conditions that may have initiated opioid use in the first place.
- Progressive social deterioration including job loss, housing instability, legal consequences, and family dissolution accelerates as opioid use disorder advances to severe classification.
How Is Fentanyl Addiction Treated?
Treating opioid use disorder involving fentanyl requires medication-assisted treatment (MAT) combined with structured behavioral therapy, addressing both the intense physical dependence and the psychological conditioning that drive compulsive use.
Medication-Assisted Treatment
FDA-approved medications for opioid use disorder represent the evidence-based standard of care, significantly reducing overdose mortality and improving treatment retention.
First-line MAT options include:
- Buprenorphine (Suboxone) is a partial mu-opioid agonist that reduces cravings and withdrawal symptoms without producing the full euphoria of fentanyl, allowing individuals to stabilize and engage in therapeutic programming.
- Naltrexone (Vivitrol) blocks mu-opioid receptors entirely as an antagonist, preventing the euphoric effects of fentanyl if relapse occurs and available as a monthly extended-release injection for improved adherence.
- Sublocade (extended-release buprenorphine injection) delivers steady-state buprenorphine levels through a monthly subcutaneous injection, eliminating daily dosing requirements and reducing diversion risk.
Behavioral Therapies
Behavioral interventions address the cognitive, emotional, and environmental factors that maintain opioid use disorder beyond physical dependence.
Effective behavioral approaches include:
- Cognitive behavioral therapy identifies and restructures the thought patterns, emotional triggers, and high-risk situations that precipitate fentanyl use, building concrete alternative coping strategies.
- Motivational interviewing enhances intrinsic motivation for change by resolving ambivalence and strengthening commitment to recovery without confrontational approaches.
- 12-step facilitation and peer support groups provide ongoing social reinforcement for abstinence and recovery, addressing the isolation that characterizes advanced opioid use disorder.
Withdrawal Management
Fentanyl withdrawal produces intensely uncomfortable but rarely life-threatening symptoms that require medical management to prevent early treatment dropout and relapse.
Withdrawal management approaches include:
- Medically supervised withdrawal using buprenorphine induction protocols stabilizes patients through the acute withdrawal phase (days 1 to 7) while establishing the foundation for ongoing MAT.
- Clonidine addresses noradrenergic withdrawal symptoms including anxiety, muscle cramping, diaphoresis, and insomnia, supplementing opioid-specific treatment approaches.
- Symptomatic medications for nausea, diarrhea, and pain management improve comfort during the acute withdrawal period and reduce the probability of return to fentanyl use to relieve withdrawal distress.
Treatment at Archangel Centers
Archangel Centers provides structured outpatient treatment for opioid use disorder through evidence-based programming and medication-assisted treatment at multiple levels of care in New Jersey.
Partial Care Program
The partial care program delivers intensive daily clinical programming from 9:00 AM to 3:15 PM, Monday through Saturday, integrating individual therapy, group sessions, and MAT services for individuals with fentanyl use disorder. Clients receive medication management with Suboxone, Naltrexone/Vivitrol, or Sublocade alongside weekly individual therapy targeting relapse prevention and recovery skills.
Intensive Outpatient Program
The intensive outpatient program provides three hours of clinical programming three to five days per week, supporting individuals who are stabilized on MAT and transitioning to lower-intensity care. IOP programming incorporates CBT, 12-step facilitation, and Smart Recovery while maintaining ongoing psychiatric and medication management oversight.
Outpatient and Virtual Programs
Outpatient services and virtual programming provide sustained recovery support through weekly therapeutic sessions, ongoing MAT, and relapse prevention programming. These levels of care support long-term opioid abstinence while accommodating work, education, and family responsibilities.
Archangel Centers offers same-day confidential assessments with insurance verification completed during the initial call.
Frequently Asked Questions
What Does Fentanyl Addiction Look Like?
Fentanyl addiction typically presents as pinpoint pupils, frequent drowsiness or “nodding off,” slowed breathing, constipation, and declining personal hygiene. Behavioral signs include social isolation, financial problems, secretive behavior, and mood cycling between sedated euphoria and anxious irritability timed to dosing schedules. Withdrawal symptoms appearing within hours of last use confirm physical dependence. (52 words)
How to Treat Fentanyl Addiction?
Treatment for fentanyl addiction combines FDA-approved medication-assisted treatment (Suboxone, Vivitrol, or Sublocade) with structured behavioral therapy including cognitive behavioral therapy and 12-step facilitation. MAT reduces cravings and withdrawal while behavioral interventions address psychological and environmental triggers. Research consistently demonstrates that combining medication with therapy produces superior outcomes compared to either approach alone. (53 words)
Is Fentanyl More Addictive Than Heroin?
Fentanyl’s 50 to 100 times greater potency compared to morphine and its rapid blood-brain barrier penetration produce stronger reinforcement conditioning than heroin. Physical dependence and tolerance develop faster with fentanyl due to more intense mu-opioid receptor activation. The extremely narrow therapeutic margin also increases overdose risk, making fentanyl the most dangerous commonly encountered opioid. (54 words)
How Many People Recover From Fentanyl Addiction?
Recovery from opioid use disorder is achievable with appropriate treatment. SAMHSA’s 2024 NSDUH reported that 74.3% of adults who perceived they ever had a substance use problem considered themselves in recovery. Medication-assisted treatment reduces opioid overdose mortality by approximately 50% and significantly improves long-term abstinence rates when maintained for a minimum of 12 months. (53 words)
What Happens During Fentanyl Withdrawal?
Fentanyl withdrawal symptoms begin within 8 to 24 hours after last use and include muscle aches, nausea, vomiting, diarrhea, insomnia, anxiety, and intense cravings. Symptoms peak between days 2 and 4. While rarely life-threatening, the severity of fentanyl withdrawal frequently drives relapse without medical support, making supervised withdrawal with buprenorphine induction the recommended approach. (54 words)
How to Help Someone Addicted to Fentanyl?
Express concern with empathy and specificity about observed changes rather than accusations. Learn about medication-assisted treatment options and local treatment providers before the conversation. Have naloxone (Narcan) available if the person is actively using, as fentanyl overdose can occur rapidly. Encourage professional assessment and offer logistical support for treatment engagement without enabling continued use. (54 words)
References
- Centers for Disease Control and Prevention. (2025). CDC reports nearly 24% decline in U.S. drug overdose deaths. https://www.cdc.gov/media/releases/2025/2025-cdc-reports-decline-in-us-drug-overdose-deaths.html
- Substance Abuse and Mental Health Services Administration. (2025). Key substance use and mental health indicators in the United States: Results from the 2024 National Survey on Drug Use and Health. https://www.samhsa.gov/data/data-we-collect/nsduh-national-survey-drug-use-and-health/national-releases/2024
- National Institute on Drug Abuse. (2024). Fentanyl drug facts. https://nida.nih.gov/publications/drugfacts/fentanyl
- Drug Enforcement Administration. (2024). Fentanyl drug fact sheet. https://www.dea.gov/factsheets/fentanyl
- Centers for Disease Control and Prevention. (2026). Drug overdose deaths in the United States, 2023-2024. https://www.cdc.gov/nchs/products/databriefs/db549.htm
- American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders (5th ed., text rev.). American Psychiatric Publishing.
- National Institute on Drug Abuse. (2024). Drug overdose deaths: Facts and figures. https://nida.nih.gov/research-topics/trends-statistics/overdose-death-rates
- Food and Drug Administration. (2023). Information about medication-assisted treatment (MAT). https://www.fda.gov/drugs/information-drug-class/information-about-medication-assisted-treatment-mat